General ENT / Surgery
Experienced Clinical and Surgical Care for Your Entire Family
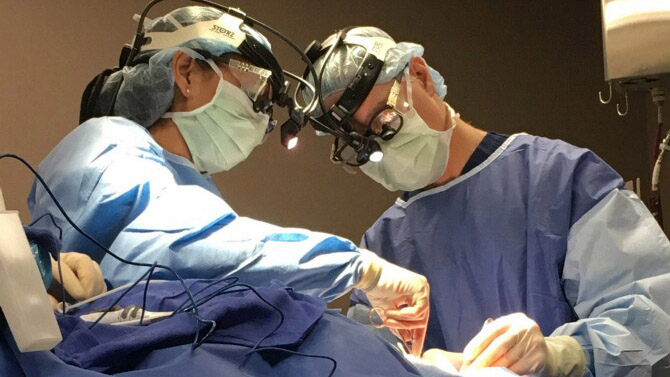
Our practice covers a wide range of diseases and conditions of the ear, nose, and throat. When surgery is recommended, we realize that there are few decisions in life more important than going to the operating room. We are experienced, Board Certified Head and Neck Surgeons, and use the latest technologies and advanced techniques while operating. However, we believe the key to a successful surgery begins with an accurate diagnosis, followed by sound clinical judgment. We will provide individualized care, counsel you on treatment options, and guide you to a successful outcome. Contact us at 204.414.1358 to schedule an appointment.
Ear FAQ
How do I remove ear wax?
First of all, what is ear wax and why do we have it?
Ear wax, or cerumen, is produced by special glands in the skin of the ear canal. It has lubricating and antibacterial properties to help protect the ear canal. A small amount is produced every day, and for most people, the ear self-cleans and a small amount is pushed out of the ear canal. For some people, there is an imbalance in the production/self-cleaning, and a build-up occurs.
How Not to Clean Your Ears
For most people, it is not necessary to clean your ears-your ears will do the job for you. As for Q-tips, the old saying applies: “Don’t put anything smaller than your elbow into your ear.” Too often, we see patients who have damaged their ear canal, or more seriously, their ear drum from using a Q-tip. Also, frequent use of peroxide or alcohol is not necessary to clean your ears. In fact, over use of these products can actually remove the protective layer of wax in your ears, causing problems such as dry itchy ears and infection of the ear canals.
How to Clean Your Ears
Over-the-counter ear wax drops, baby oil, and mineral oil can be used to help soften wax. We recommend a few drops twice a day for 3-4 days. Initially, the drops may cause your ears to feel “plugged up.” On the fourth day, you can use a syringe of warm water or water while showering to irrigate your ears. However, for dense impactions, the over-the-counter treatment is unlikely to remove the wax. If this is the case, call Dr. McCool or Dr. Bhuta to schedule an appointment.
What are chronic ear infections?
If a child has an ear infection, it is most likely otitis media. This is an infection of the middle ear, which is the space deep to the ear drum. The Eustachian tube, which connects the nose to the middle ear space, helps to keep the middle ear ventilated and dry. Sometimes in children, the Eustachian tube does not function well, and fluid can accumulate in the middle ear. An infection can then develop within this fluid. A child may have acute recurring infections that resolve, or a chronic condition that does not respond to antibiotics.
The most common symptom is ear pain, that is often quite severe. Infants can have a lot of difficulty trying to sleep, and overall can be irritable. If your child has had three episodes of otitis media requiring antibiotics, consider a visit with Dr. McCool or Dr. Bhuta. They are on staff physicians at Children’s Hospital, and if placing ear tubes is recommended, they can perform the procedure at the Children’s Outpatient Surgery Center.
How do I know if my child needs tubes in his/her ears?
The middle ear space, which is the space deep to the eardrum, is connected to the nose via the Eustachian tube. It is a ventilation system to keep the middle ear space dry. Sometimes in children, the Eustachian tube does not function well, and fluid can accumulate in the middle ear. An infection can then develop within this fluid.
A child may have acute recurring infections that require multiple rounds of antibiotics or a chronic condition that does not respond to antibiotics. In either situation, your child may be a candidate for having ventilation tubes placed through the eardrums. This operation called a bilateral myringotomy with tubes, allows the middle ear space to ventilate until the Eustachian tubes fully mature. The tubes usually stay in place for 12-18 months, and will eventually fall out of the eardrum and out of the ear without further treatment. The many benefits of having tubes include, 1) a significant reduction in the number of ear infections, oftentimes to zero; 2) allowing an infection to drain out of the ear, thus reducing the pain and possible complications associated with an ear infection; and 3) access to middle ear space so that an infection can be treated directly with topical antibiotic drops.
Contact our office to discuss a treatment plan for your child’s recurrent ear infections. If the placement of ventilation tubes is recommended, Dr. McCool and Bhuta are on-staff physicians at Children’s Hospital and can perform the procedure at the Children’s Outpatient Surgery Center.
Nose FAQ
What should I do if I am having a nosebleed?
The source of most nosebleeds (epistaxis) is the front part of the nasal septum, the midline structure which divides the nasal passage into a left and right side. The septum contains many superficial blood vessels that can bleed spontaneously or are injured by trauma to the nose. Nosebleeds coming from the front of the nose (anterior nosebleeds) often begin with a flow of blood out of one nostril when the patient is sitting or standing.
Anterior nosebleeds are common in dry climates or during the winter months when dry, heated indoor air dehydrates the nasal membranes. Dryness may result in crusting, cracking, and bleeding. This can be prevented by placing a light coating of petroleum jelly or an antibiotic ointment on the end of a fingertip and then rub it inside the nose, especially on the middle portion of the nose (the septum).
How do I stop an anterior nosebleed?
- Stay calm. Anxiety/excitement can elevate blood pressure which will cause more bleeding.
- Sit up to keep your head higher than the level of your heart
- Lean slightly forward so the blood won’t drain in the back of the throat.
- Using the thumb and index finger, pinch the soft tissue of the nose in order to apply pressure to the septum for five minutes. Pinching the hard, bony part of the upper nose will not help to stop a nose bleed. If the bleeding does not stop in five minutes, you can place a cotton ball soaked with Afrin or Neo-Synephrine spray into the nostril and then apply pressure.
Sometimes the source of a nosebleed is deep inside the nose, and the bleeding can flow down the back of the throat, even if you are seated or standing. This is a posterior nose bleed, and since they are more difficult to control, you will likely need the help of Dr. McCool or Dr. Bhuta. We will see patients immediately during office hours for an active nosebleed, but you can use Afrin or Neosynephrine to slow down the bleeding. Posterior nosebleeds are more likely to occur in older people, persons with high blood pressure, and in cases of injury to the nose or face.
Call our office to schedule an appointment.
What is a deviated septum?
The nasal septum is the midline supporting wall inside your nose, dividing the nasal cavity into halves. The front portion of this natural partition is firm but bendable, just like the tip of your nose, and is made mostly of cartilage. The deeper, more posterior part of the septum is a thin wall of bone.
Many patients will have a septum that is slightly off-center but is usually asymptomatic. A deviated septum occurs when the septum is severely shifted away from the midline. The most common symptom is nasal obstruction- difficulty breathing through your nose on one or both sides. In some cases the deviated septum can interfere with the drainage of the sinuses, resulting in repeated sinus infections.
Other symptoms include frequent nosebleeds, facial pressure and pain, and mouth breathing.
If the nasal obstruction caused by the deviated septum does not respond to medication, then septoplasty is the preferred treatment to correct a deviated septum. This procedure is performed in the operating room and may remove the deviated portion of the septum or reposition the septum in the middle.
Drs. McCool and Bhuta are Board Certified Otolaryngologists-Head and Neck Surgeons, each with over 15 years of experience. If you are suffering from nasal congestion, facial pressure, and pain, or frequent nosebleeds, then you may have a deviated septum. Contact McCool and Bhuta Ear Nose and Throat Specialists to schedule your evaluation.
What is snoring?
Snoring is a noise during sleep made by the vibration of the soft tissue in the upper airway- your mouth, nose and the back of your throat. It occurs mostly when we inhale (breath in). As we fall asleep, the muscles of our tongue and throat relax. When you inhale, the airflow can cause this tissue to flutter, resulting in a variety of snoring sounds. Quite often, snoring, especially if it is loud, is an indication of a more serious problem called Obstructive Sleep Apnea, or OSA. OSA is the periodic obstruction of the airway during sleep, potentially causing a variety of health problems such as high blood pressure and heart arrhythmias. It also interferes with the normal sleep stages, which prevents deep, restful sleep. Frequent nighttime trips to the bathroom, morning headaches, and excessive daytime sleepiness are all signs of possible OSA.
If you or your bed partner has snoring, contact McCool and Bhuta Ear Nose and Throat Specialists for a complete evaluation, and let us help you to get the restful sleep that you deserve.
Throat FAQ
What is reflux?
Gastro-Esophageal Reflux Disease, or GERD, occurs when stomach contents flow back into the esophagus and throat. When this reflux irritates the throat and voice box, it is called Laryngo-Pharyngeal –Reflux, or LPR. Heartburn is an obvious symptom, but about 50% of people with reflux may not have heartburn, which is called “Silent Reflux.”
The most common symptom of LPR is a chronic dry cough and throat clearing. Other symptoms include
- Thick mucus in the throat that is difficult to clear
- Difficulty swallowing, or dysphagia
- A “lump” in the throat
- Hoarseness
Tips to reduce GERD and LPR include avoiding foods that promote reflux, such as caffeine, alcohol, spicy foods, citric acid drinks, and cough drops and mints. *Remember, once the symptoms of LPR occur, it can take several weeks for them to resolve, even with dietary changes. However, if dietary measures do not relieve your symptoms, contact Drs. McCool and Bhuta for an evaluation and treatment plan.
What is causing my hoarseness?
Your vocal cords are the structures in your larynx (“voice-box”) that produce the sounds of speech. When you breathe, the vocal cords are in an open “V” shape, allowing air to pass into and out of your lungs. When you speak, the vocal cords close, and as air from your lungs passes through the cords, the cords vibrate, like the reed in a clarinet or saxophone. This produces the initial sound of your voice, which is then modified by the structures in your throat and mouth. When your vocal cords are not vibrating correctly, your voice is hoarse, and sounds rough or raspy. Other voice problems include a change of pitch, loss of vocal range and endurance, and discomfort when speaking or singing for longer periods of time.
One of the most common causes of hoarseness is an upper respiratory infection. During an infection, the throat and larynx are inflamed, irritated, and swollen, which interferes with the natural vibration of the vocal cords. Almost always, hoarseness associated with an upper respiratory infection will resolve in 2-3 weeks. However, if your voice does not return to normal in 3-4 weeks, you should be evaluated by Dr. McCool or Dr. Bhuta to rule out a more serious problem. Other causes of hoarseness include a benign growth on the cords, such as nodules or a polyp, and reflux. *Any voice changes in a patient with a smoking history should be evaluated as soon as possible.
Six Tips To Identify Voice Problems
Ask yourself the following questions to determine if you have hoarseness/voice problem:
- Has your voice become hoarse or raspy?
- Does your throat often feel raw, achy, or strained?
- Does talking require more effort?
- Do you find yourself repeatedly clearing your throat?
- Do people regularly ask you if you have a cold when in fact you do not?
- Have you lost your ability to hit some high notes when singing?
A wide range of problems can cause hoarseness/voice changes. Contact McCool and Bhuta Ear Nose and Throat Specialists today to discuss your vocal problems with Dr. McCool or Dr. Bhuta.
Surgery FAQ
What is Balloon Sinuplasty?
Balloon Sinuplasty is a procedure that relieves the congestion and facial pressure and pain associated with chronic sinusitis. It is used by Dr. McCool and Dr. Bhuta to safely and effectively treat chronic sinusitis patients who are seeking relief from these uncomfortable and painful symptoms of sinusitis.
Balloon Sinuplasty is similar to angioplasty, whereby balloons are used to open blocked arteries. An FDA-approved procedure, is less invasive than traditional sinus surgery, and it allows most patients to return to normal activities within two to three days. With Balloon Sinuplasty, a specially‐designed catheter is inserted into the nose, and then into the narrow channels that drain the sinuses. A small balloon is slowly inflated, which widens and restructures the walls of the sinus passage. The trapped mucus within the sinus is drained, but the natural structures within the nose and sinuses are preserved. This allows for minimal to no bleeding or scarring, which in traditional sinus surgery can lead to further blockage of the sinuses.
Balloon Sinuplasty can be performed in the office or as an outpatient procedure and is covered by most insurance plans, including Medicare. If you suffer from chronic sinusitis and are not responding well to medications, contact McCool and Bhuta Ear Nose and Throat Specialists to determine if Balloon Sinuplasty is right for you.
What is a tonsillectomy/adenoidectomy?
Unfortunately, there may be a time when medical therapy (antibiotics) fails to resolve the chronic tonsil infections that affect your child. In other cases, your child may have enlarged tonsils, causing loud snoring, upper airway obstruction, and other sleep disorders. The best treatment for both of these conditions may be the removal of the tonsils and adenoids.
The procedure to remove the tonsils is called a tonsillectomy; excision of the adenoids is an adenoidectomy. Both are usually performed concurrently; hence the procedure is known as a tonsillectomy and adenoidectomy, or T&A. The American Academy of Otolaryngology-Head and Neck Surgery recommends that children who have three or more tonsil infections in a year undergo a tonsillectomy and adenoidectomy. This procedure is also indicated for a child with loud snoring and obstructions when they are sleeping. Tonsillectomy and adenoidectomy is an outpatient surgical procedure lasting about twenty minutes and performed under general anesthesia. Usually, a child will remain at the hospital or surgery center for 2-3 hours after surgery for observation. For some children, overnight observation is required.
Dr. McCool and Dr. Bhuta are Board Certified physicians for the Children’s Hospital of Alabama and have taken care of children in the Birmingham area for the past 15 years. If your child suffers from repeated throat and tonsil infections or has loud snoring with restless sleep, contact McCool and Bhuta Ear Nose and Throat Specialists for an evaluation.
What is thyroid surgery?
The thyroid gland is located in the lower neck. It has a left and right lobe, connected by a band of thyroid tissue called the isthmus, which crosses the trachea (windpipe). The thyroid gland secretes hormones that are responsible for regulating your metabolism.
What is a thyroid disorder?
Diseases of the thyroid gland are very common, affecting millions of Americans. The most common thyroid problems are:
- Hyperthyroidism-an overactive gland that is secreting too much thyroid hormone(e.g., Graves’ disease, toxic adenoma or toxic nodular goiter)
- Hypothyroidism-a gland that is not secreting enough thyroid hormone (e.g., Hashimoto’s thyroiditis)
- Thyroid enlargement-commonly called a goiter. This can be caused by either an overactive or underactive gland. A thyroid gland may have a single enlarged nodule, or multiple smaller nodules.
What is thyroid surgery?
Thyroid surgery is an operation to remove a portion or all of the thyroid gland. Once removed, the gland is examined by pathologists to determine the type of thyroid disorder. Sometimes, a thyroid cancer is discovered, and additional surgery may be required. Dr. McCool and Dr. Bhuta are Board Certified Head and Neck Surgeons, each with nearly 20 years of experience in thyroid surgery. Call us today to schedule an appointment at McCool and Bhuta Ear Nose and Throat Specialists.
Contact McCool and Bhuta
for more information or to schedule an appointment.
205.414.1368

3055 Independence Drive | Homewood, AL 35209
205.414.1368 | info@entbirmingham.com

3055 Independence Drive
Homewood, AL 35209
205.414.1368
info@entbirmingham.com